
Management of Diabetes Perioperative
The increasing prevalence of diabetes mellitus results in an increasing number of diabetic patients undergoing surgery.


The increasing prevalence of diabetes mellitus results in an increasing number of diabetic patients undergoing surgery.
The occurrence of surgery in diabetic patients, highlights the importance of stress, hyperglycaemia, diabetes management, optimal glycaemic control, and the importance of a multidisciplinary team approach in management of patients during the perioperative stages.
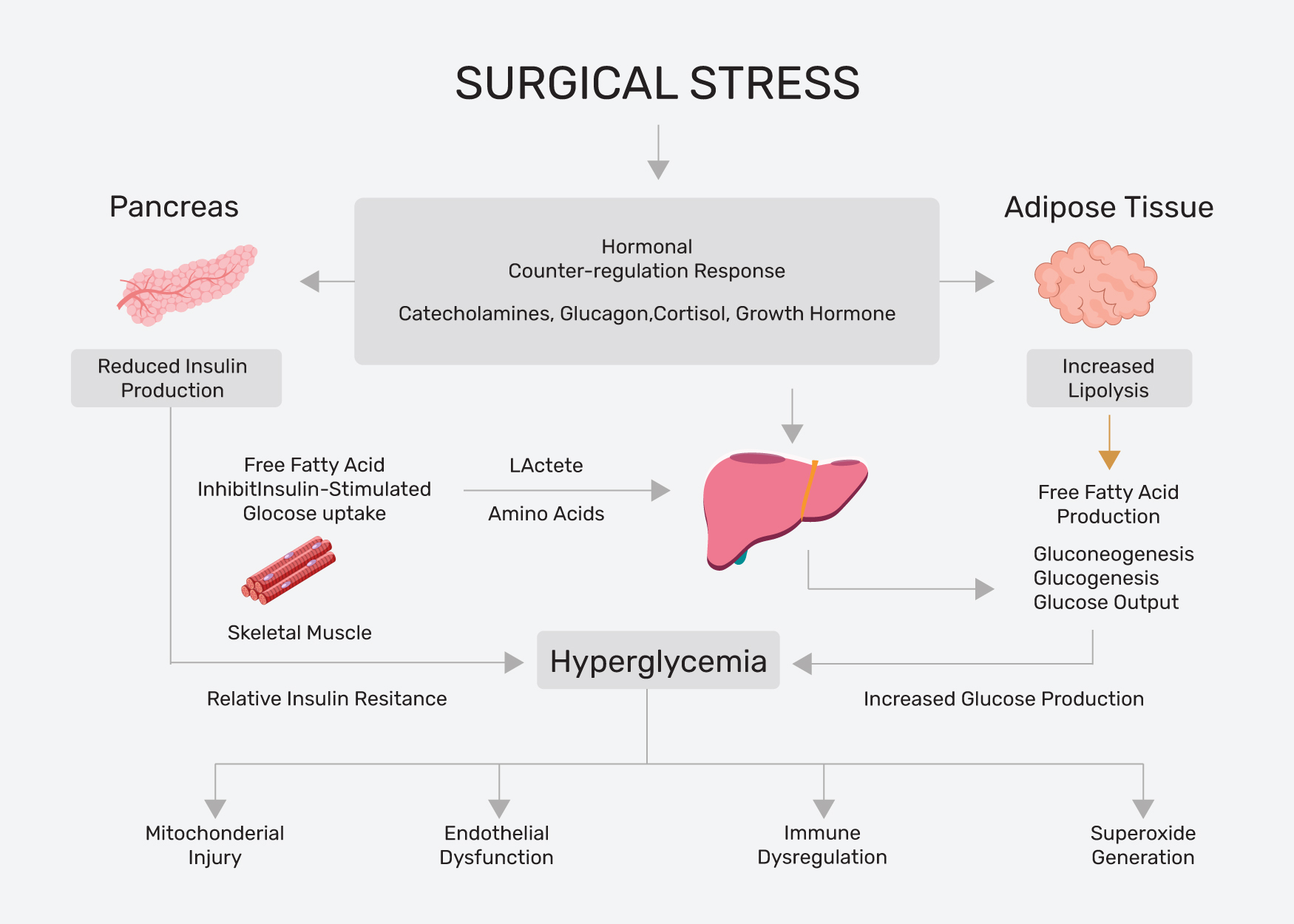
The stress of surgery, anesthesia and illness increases secretion of counter-regulatory hormones (cortisol, glucagon, growth hormone, catecholamines), which in turn causes decreased insulin secretion, increased insulin resistance, decreased peripheral utilization of glucose, increased lipolysis, and proteolysis. Therefore, gluconeogenesis and glycogenolysis increase, which subsequently results in worsening hyperglycemia termed as stress hyperglycemia[1].
Preoperatively, it is crucial to have an individualized care plan with clear perioperative pathway, planning and proper communication among the health care providers and patient. This further aids in improving the perioperative outcome.
Usually, the perioperative process for people with diabetes begins with a referrall that should contain the following information (2)
The perioperative period is divided into three phases: Preoperative, Intraoperative and Postoperative
In this phase the health care team should start putting a care plan evaluating the diabetic patients’ history which includes type of diabetes, management, glycemic control, complications, hypoglycemia risks, and previous surgeries. A preoperative haemoglobin A1c (HbA1c) should be checked, as mmultiple studies have looked at the association of HbA1c and surgical outcomes and insulin should be initiated if blood glucose is > 180 mg/dl.(2)
Minimize fasting period, maintain CBG (capillary blood glucose) and clear diabetic management handover.
In the postoperative care it is important to continue close glucose monitoring with CBG (capillary blood glucose). Correctional subcutaneous rapid-acting insulin doses are provided for CBG greater than 180 mg/dl and should be referred to the Endocrinology team. Upon stabilisation and oral intake tolerance, the patient can be discharged with proper education about all medication changes, future diabetes care plan and emphasizing the importance of diabetes self-management. (3)

Due to minimal to no pancreatic beta-cell function, type 1 diabetics should always have a basal supply of insulin (even if nothing by mouth), either subcutaneously or intravenously to avoid diabetic ketoacidosis.
As using insulin pump has increased especially in type 1 diabetes, the use of insulin pumps in the hospital setting during the pre-/postoperative period must be guided by clear institutional policies and the patient’s ability to manage the pump. (4)
A hospital must work with a multidisciplinary team approach to create appropriate protocols for hyperglycemia screening, monitoring, and treatment to minimize complications and ensure better care for patients.
[1] Duggan, E. W., Carlson, K., & Umpierrez, G. E. (2017). Perioperative hyperglycemia management: an update. Anesthesiology, 126(3), 547-560.
[2] Dogra P, Jialal I. Diabetic Perioperative Management. 2022 Jun 19. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan–. PMID: 31082009.
[3] Khan, N. A., Ghali, W. A., & Cagliero, E. (2016). Perioperative management of blood glucose in adults with diabetes mellitus. UpToDate. Waltham, MA (Accessed on 1/15/2017).
[4] CPOC Diabetes Surgery Guideline March 2021 https://abcd.care/sites/abcd.care/files/site_uploads/CPOC_Diabetes_Surgery_Guideline_March_2021.pdf
For the next FUH Medical Review
©2021 Fakeeh University Hospital. All Rights Reserved
To FUH Medical Review